Can Methylation affect Immune Function?The immune system protects the body from external threats such as viruses, bacteria, parasites, and chemicals. The key to the functioning of the immune system is its ability to differentiate between self (healthy tissue) and non-self. The immune system consists of several subsystems all working together as a unit to protect the body. It can be split into the innate immunity which consists of non-specific defence mechanisms such as the skin; and specific immunity consisting of specialized cells and processes that remove harmful and foreign microbes or chemicals. The specific immunity can be further divided into the humoral immunity where B-cells are found; and cellular immunity which is orchestrated by T-cells.
What are autoimmune diseases?Disorders of the immune system can be described as an over activity or low activity of the immune system. The more well-known immune system disorders are the over activity type and are known as autoimmune diseases. Autoimmune diseases occur when there is an error in the immune system’s ability to differentiate between healthy self-cells and harmful non-self-cells or chemicals; in this instance the immune system will begin to attack healthy tissue instead of fighting infections. The most common autoimmune diseases include Rheumatoid arthritis, systemic lupus erythematosus, inflammatory bowel disease, multiple sclerosis, type 1 diabetes, Guillain-Barre syndrome, psoriasis and Grave’s disease.
EpigeneticsStudies have implicated epigenetic influences with regards to the formation of autoimmunity. Epigenetics is a relatively new field of study, and research is still in its infancy; what is known is that epigenetics describes the changes in gene expression brought about by environmental influences without affecting the underlying genomic sequence. The updated definition of epigenetics is proposed by Bird et al. who quotes: “the structural adaptation of chromosomal regions so as to register, signal or perpetuate altered activity states”; this statement helps us understand the role epigenetic mechanisms play in influencing cellular response to environmental stimuli; and with regards to autoimmune diseases we see how this definition is closely related. Epigenetics consists of three groups, they are cytosine genomic DNA methylation, modification of various sidechain positions of histone proteins, nucleosome positioning and noncoding RNAs.
DNA methylationDNA methylation occurs in various regions of the genome and can be seen during embryogenesis, cellular differentiation and tissue-specific development. DNA methylation operates at varying rates depending on the cell type, and its two main functions are either to methylate or de-methylate a region of DNA. Methylation is thought to cause repression of a gene while de-methylation enables the activation of a gene, together these processes contribute to the normal regulatory functions and any breakdown in these processes may ultimately lead to disease.
The enzymes responsible for DNA methylation belong to the DNA methyltransferase (DNMTs) family. There are five enzymes that mediate methylation, they are: DNMT1, DNMT2, DNMT3a, DNMT3b and DNMT3L, and their function is to donate a methyl group to the 5’- carbon of cytosine. DNMT3a and DNMT3b are primarily found to operate during embryonic development, whilst DNMT1 is responsible for methylation during DNA replication, due to the formation hemimethylated sites; DNMT2 methylates transfer RNA.
DNA demethylation counteracts methylation and can be active or passive. Passive demethylation is brought about by the inhibition of DNMTs, this is induced by certain therapeutic drugs that aim to reduce hypermethylation. Active demethylation occurs during cell differentiation and plays an important role in the activation of immune cells. Studies have shown that DNA methylation has a critical role in maintaining T-cell function. Once DNA methylation levels in T-cells reduce i.e. they demethylate, the T-cells may become autoreactive resulting in autoimmunity. Studies have also shown that the autoimmune diseases systemic lupus erythematosus (SLE) and rheumatoid arthritis (RA) have been found to have hypomethylation as a trait
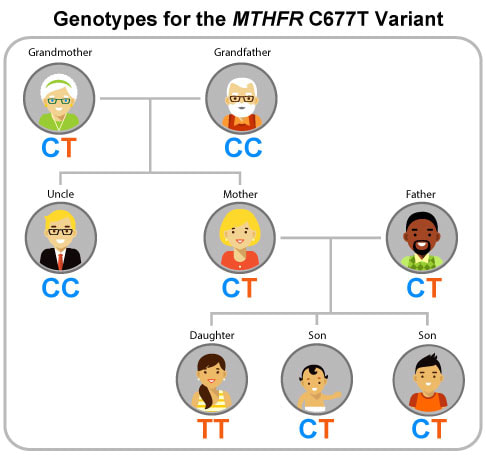
MTHFR deficiency and autoimmune conditionsThe MTHFR gene can be indirectly linked to the formation of autoimmune diseases, this may be evident in the MTHFR C677T polymorphism. An impairment in DNA methylation can occur if there is a deficiency in the MTHFR gene. A deficiency in the MTHFR gene may result in a reduction in the conversion of 5, 10-methylenetetrahydrofolate to 5-methyltetrahydrofolate which is used in the methionine cycle to generate S-adenosyl-L-methionine (SAM), the primary methyl group donor for most biological methylation reactions. We have seen the important role methylation plays in the normal functioning of T-Cells in the immune system and the prevention of autoimmunity.
ConclusionTo limit the effect of overactive autoimmunity in those who are susceptible we can optimise methylation, reduce inflammation and ensure that gut function is optimal.
What are autoimmune diseases?Disorders of the immune system can be described as an over activity or low activity of the immune system. The more well-known immune system disorders are the over activity type and are known as autoimmune diseases. Autoimmune diseases occur when there is an error in the immune system’s ability to differentiate between healthy self-cells and harmful non-self-cells or chemicals; in this instance the immune system will begin to attack healthy tissue instead of fighting infections. The most common autoimmune diseases include Rheumatoid arthritis, systemic lupus erythematosus, inflammatory bowel disease, multiple sclerosis, type 1 diabetes, Guillain-Barre syndrome, psoriasis and Grave’s disease.
EpigeneticsStudies have implicated epigenetic influences with regards to the formation of autoimmunity. Epigenetics is a relatively new field of study, and research is still in its infancy; what is known is that epigenetics describes the changes in gene expression brought about by environmental influences without affecting the underlying genomic sequence. The updated definition of epigenetics is proposed by Bird et al. who quotes: “the structural adaptation of chromosomal regions so as to register, signal or perpetuate altered activity states”; this statement helps us understand the role epigenetic mechanisms play in influencing cellular response to environmental stimuli; and with regards to autoimmune diseases we see how this definition is closely related. Epigenetics consists of three groups, they are cytosine genomic DNA methylation, modification of various sidechain positions of histone proteins, nucleosome positioning and noncoding RNAs.
DNA methylationDNA methylation occurs in various regions of the genome and can be seen during embryogenesis, cellular differentiation and tissue-specific development. DNA methylation operates at varying rates depending on the cell type, and its two main functions are either to methylate or de-methylate a region of DNA. Methylation is thought to cause repression of a gene while de-methylation enables the activation of a gene, together these processes contribute to the normal regulatory functions and any breakdown in these processes may ultimately lead to disease.
The enzymes responsible for DNA methylation belong to the DNA methyltransferase (DNMTs) family. There are five enzymes that mediate methylation, they are: DNMT1, DNMT2, DNMT3a, DNMT3b and DNMT3L, and their function is to donate a methyl group to the 5’- carbon of cytosine. DNMT3a and DNMT3b are primarily found to operate during embryonic development, whilst DNMT1 is responsible for methylation during DNA replication, due to the formation hemimethylated sites; DNMT2 methylates transfer RNA.
DNA demethylation counteracts methylation and can be active or passive. Passive demethylation is brought about by the inhibition of DNMTs, this is induced by certain therapeutic drugs that aim to reduce hypermethylation. Active demethylation occurs during cell differentiation and plays an important role in the activation of immune cells. Studies have shown that DNA methylation has a critical role in maintaining T-cell function. Once DNA methylation levels in T-cells reduce i.e. they demethylate, the T-cells may become autoreactive resulting in autoimmunity. Studies have also shown that the autoimmune diseases systemic lupus erythematosus (SLE) and rheumatoid arthritis (RA) have been found to have hypomethylation as a trait
MTHFR deficiency and autoimmune conditionsThe MTHFR gene can be indirectly linked to the formation of autoimmune diseases, this may be evident in the MTHFR C677T polymorphism. An impairment in DNA methylation can occur if there is a deficiency in the MTHFR gene. A deficiency in the MTHFR gene may result in a reduction in the conversion of 5, 10-methylenetetrahydrofolate to 5-methyltetrahydrofolate which is used in the methionine cycle to generate S-adenosyl-L-methionine (SAM), the primary methyl group donor for most biological methylation reactions. We have seen the important role methylation plays in the normal functioning of T-Cells in the immune system and the prevention of autoimmunity.
ConclusionTo limit the effect of overactive autoimmunity in those who are susceptible we can optimise methylation, reduce inflammation and ensure that gut function is optimal.
It might look like a curse word at first glance, but it actually refers to a relatively common genetic mutation. MTHFR stands for methylenetetrahydrofolate reductase. It's getting attention due to a genetic mutation that may lead to high levels of homocysteine in the blood and low levels of folate and other vitamins.
People with MTHFR mutations may want to avoid foods that contain the synthetic form of folate, namely folic acid
What do you do if you have the MTHFR gene mutation?
Natural treatments for MTHFR mutation symptoms
Natural treatments for MTHFR mutation symptoms
- Consume more folate and vitamin B12. Consuming more folate in your diet may aid with methylation. ...
- Support detoxification. ...
- Minimize alcohol intake. ...
- Manage your stress with lifestyle changes. ...
- Check your supplements. ...
- Heal any underlying digestive issues.
Normal Function
Collapse SectionThe MTHFR gene provides instructions for making an enzyme called methylenetetrahydrofolate reductase. This enzyme plays a role in processing amino acids, the building blocks of proteins. Methylenetetrahydrofolate reductase is important for a chemical reaction involving the vitamin folate (also called vitamin B9). Specifically, this enzyme converts a form of folate called 5,10-methylenetetrahydrofolate to a different form of folate called 5-methyltetrahydrofolate. This is the primary form of folate found in blood, and is necessary for the multistep process that converts the amino acid homocysteine to another amino acid, methionine. The body uses methionine to make proteins and other important compounds.
Collapse SectionThe MTHFR gene provides instructions for making an enzyme called methylenetetrahydrofolate reductase. This enzyme plays a role in processing amino acids, the building blocks of proteins. Methylenetetrahydrofolate reductase is important for a chemical reaction involving the vitamin folate (also called vitamin B9). Specifically, this enzyme converts a form of folate called 5,10-methylenetetrahydrofolate to a different form of folate called 5-methyltetrahydrofolate. This is the primary form of folate found in blood, and is necessary for the multistep process that converts the amino acid homocysteine to another amino acid, methionine. The body uses methionine to make proteins and other important compounds.
Polymorphisms in the MTHFR gene can alter or decrease the activity of methylenetetrahydrofolate reductase, leading to a mild increase of homocysteine in the blood (hyperhomocysteinemia). The two MTHFR gene polymorphisms that are the most common and the most frequently studied are 677C>T and a change that replaces the nucleotide adenosine with the nucleotide cytosine at position 1298 (written as 1298A>C).
An increase in homocysteine levels caused by MTHFR gene polymorphisms have been studied as possible risk factors for a variety of common conditions. These include high blood pressure (hypertension), blood clots, pregnancy loss, psychiatric disorders, and certain types of cancer. Research indicates that individuals who have the 677C>T polymorphism on both copies of the MTHFR gene have an increased risk of developing vascular disease, including heart disease and stroke. The 677C>T polymorphism has also been suggested as a risk factor for cleft lip and palate, a birth defect in which there is a split in the upper lip and an opening in the roof of the mouth.
Studies of MTHFR gene variations in people with these disorders have had mixed results, with associations found in some studies but not in others. Therefore, the role that changes in the MTHFR gene play in these disorders remains unclear. It is likely that additional factors influence the processing of homocysteine and that variations in homocysteine levels play a role in whether a person develops any of these conditions. A large number of genetic and environmental factors, most of which remain unknown, likely determine the risk of developing most common complex conditions.
An increase in homocysteine levels caused by MTHFR gene polymorphisms have been studied as possible risk factors for a variety of common conditions. These include high blood pressure (hypertension), blood clots, pregnancy loss, psychiatric disorders, and certain types of cancer. Research indicates that individuals who have the 677C>T polymorphism on both copies of the MTHFR gene have an increased risk of developing vascular disease, including heart disease and stroke. The 677C>T polymorphism has also been suggested as a risk factor for cleft lip and palate, a birth defect in which there is a split in the upper lip and an opening in the roof of the mouth.
Studies of MTHFR gene variations in people with these disorders have had mixed results, with associations found in some studies but not in others. Therefore, the role that changes in the MTHFR gene play in these disorders remains unclear. It is likely that additional factors influence the processing of homocysteine and that variations in homocysteine levels play a role in whether a person develops any of these conditions. A large number of genetic and environmental factors, most of which remain unknown, likely determine the risk of developing most common complex conditions.
At least 40 mutations in the MTHFR gene have been identified in people with homocystinuria, a disorder in which the body is unable to process homocysteine and methionine properly. People with this condition often develop eye problems, abnormal blood clotting, skeletal abnormalities, and learning problems. Most of the mutations that cause homocystinuria change single amino acids in methylenetetrahydrofolate reductase. These changes impair the function of the enzyme, and some cause the enzyme to be turned off (inactivated). Other mutations lead to the production of an abnormally small, nonfunctional version of the enzyme. Without functional methylenetetrahydrofolate reductase, homocysteine cannot be converted to methionine. As a result, homocysteine builds up in the bloodstream, and the amount of methionine is reduced. Some of the excess homocysteine is excreted in urine (homocystinuria). Researchers have not determined how altered levels of homocysteine and methionine lead to the various health problems affecting multiple parts of the body in people with homocystinuria.